Equine Light Therapy
Helping your horse heal with the speed of light
What is Phovia Light Therapy?
Phovia is a new, reliable technology using fluorescent light energy to aid in managing inflammation and bacterial infections. The technology is photobiomodulation via fluorescent light energy. It is recommended for skin infections, wounds, and chronic and recurrent inflammatory skin conditions. The therapy promotes tissue healing, reduces inflammation, and supports collagen production.
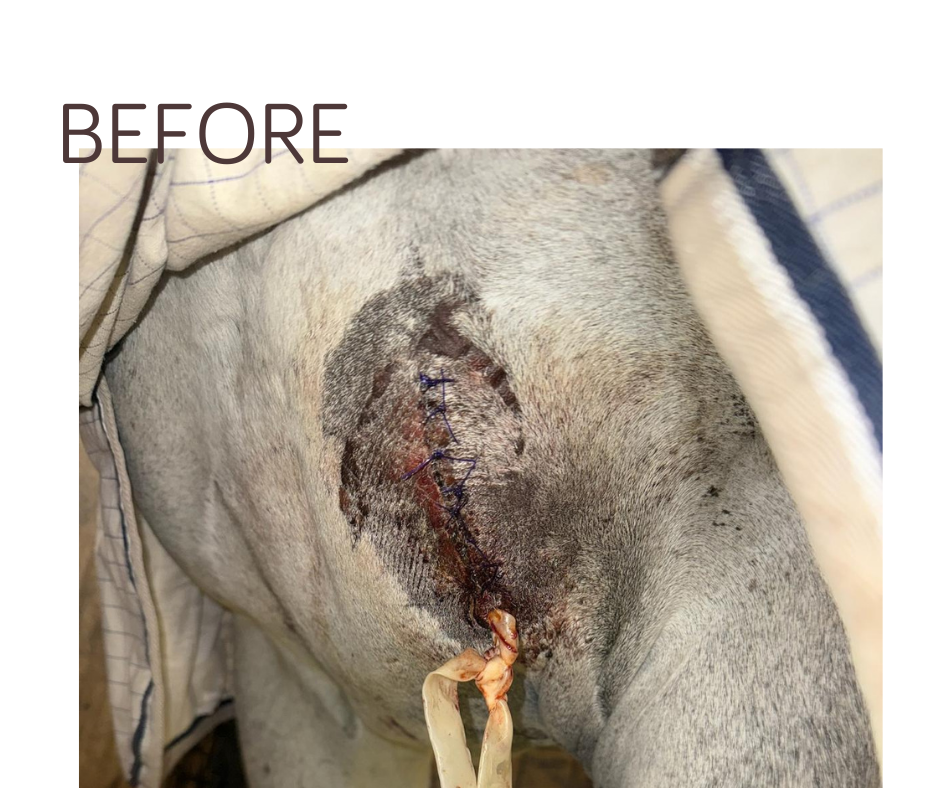
A Tool in PetDerm’s Healing Kit
If your horse is experiencing reoccuring infections or resistance to routine treatments, Phovia light therapy can be a crucial aid to healing the skin. It is a supportive therapeutic approach that reduces the length of systemic antibiotic use in the treatment of resistant infections. Most importantly, it often provides your horse with more immediate ad direct relief.
Multiple Phovia treatments are necessary to achieve optimal healing, as the therapy works by gradually stimulating the skin’s natural repair processes over time. Regular sessions ensure sustained improvement, reducing inflammation, and promoting consistent tissue regeneration for better long-term results.
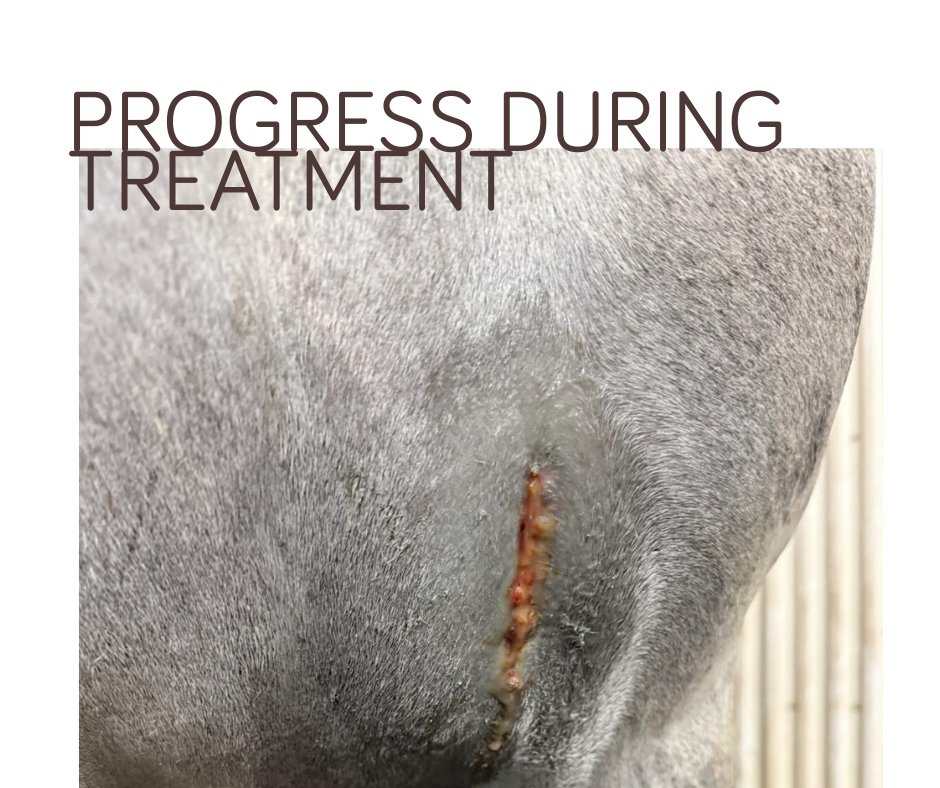
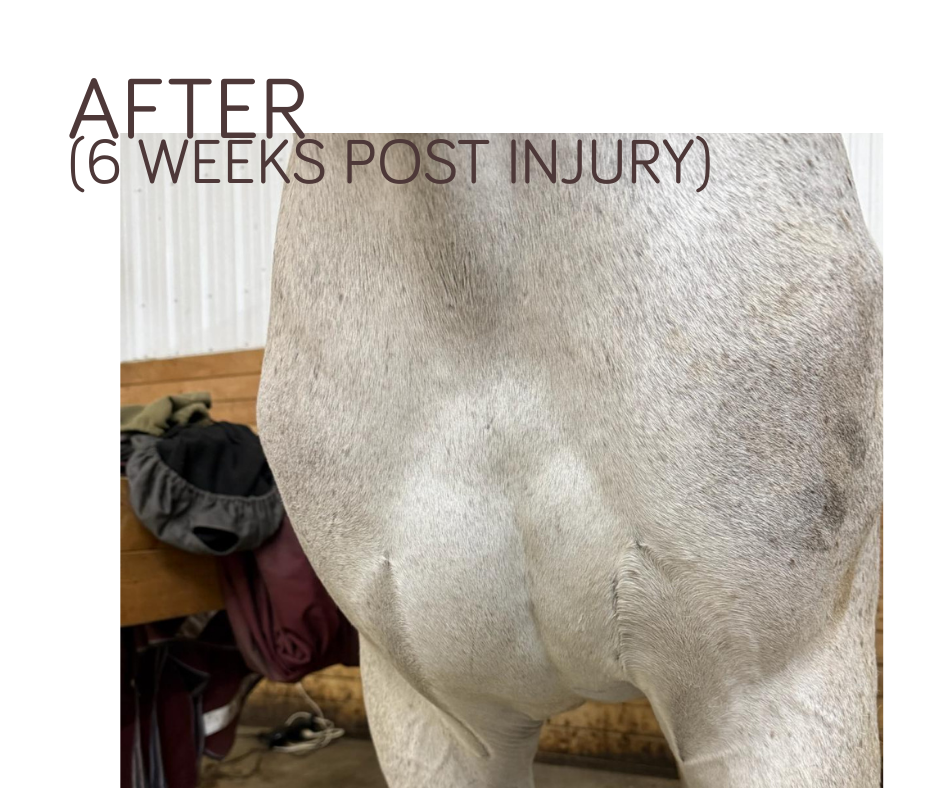
When to Consider Equine Light Therapy
PetDerm’s can help speed up your horse’s healing efforts with a:
- Injury or recent surgery
- Reoccurent or antibiotic resistant skin infections
A dermalogical consultation with PetDerm’s equine team will provide you whether this treatment is suitable for your horse’s pathway to recovery.
Equine Dermatology Referral Process
At PetDerm equine services, we prioritize your horse’s comfort and well-being. Simply ask your veterinarian to complete our online referral form, and once it’s submitted, a member of the PetDerm team will reach out to guide you through the next steps.
Appointments are scheduled offsite, and we collaborate with your primary veterinarian to tailor each appointment to your horse’s specific needs.

Frequently Asked Questions
Some horses will require ongoing management, while others may experience various periods of improvement. PetDerm will work closely with your primary veterinarian to create a responsive and malluable treatment plan to match your horse’s current symptoms.
Autoimmune skin conditions are usually managed rather than cured. With the right treatment plan, many horses can remain comfortable, and active. Early detection can help slow the progression of the disease.
They can be uncomfortable or painful, especially when lesions are inflamed or slow to heal. Proper management focuses on reducing discomfort and preventing complications. PetDerm’s dermatological veterinarian provides an individualized management plan to improve the overall quality of life for your horse.
Yes! Reducing exposure to dust, mold, and airborne irritants in barns and stables is one of the most effective ways to manage equine asthma. Especially in Alberta’s harsh climate where horses spend more time indoors during the winter months.
Equine asthma is often managed long-term rather than a curable disease. With appropriate environmental control and allergy management, many horses can have a comfortable and improved quality of life. PetDerm’s goal is the provide you and your primary veterinarian with a sustainable long-term management plan.
No. Equine asthma is not caused by bacteria or viruses. It is an inflammatory condition often linked to allergies and environmental exposure, which is why antibiotics are not typically effective. A dermatologic assessment may be necessary to evaluate the underlying cause and early on intervention to slow the progression of the disease.
Early signs may include occasional coughing, reduced stamina, slower recovery after exercise, or subtle breathing changes. These signs can be easy to miss at first but may worsen over time without medical intervention. If you suspect that your horse has enviornmental allergies, ask your primary veterinarian for a referral today!
In many horses, equine asthma is part of a broader allergic response. The same allergens that cause skin problems can also affect the airways, which is why some horses experience both skin and respiratory symptoms.
Learn more about PetDerm’s intradermal allergy testing.
Yes. Adjustments such as improving regular hygiene, reducing moisture exposure, managing insects, or modifying stable conditions can play an important role in preventing flare-ups and supporting treatment success.
Some equine skin conditions can be ongoing and require long-term management rather than a one-time treatment. With proper care, many horses can remain comfortable and active even with chronic skin disease.
They can. Skin pain, irritation, or lesions—especially in areas under tack or around the legs—can cause discomfort, behavioral changes, and reduced willingness to work. Managing skin disease helps support both comfort and performance.
You should consider a dermatology veterinary evaluation if a skin problem:
- Persists longer than expected
- Keeps returning after treatment
- Causes significant itching or discomfort
- Spreads or worsens over time
- Interferes with riding, training, or daily comfort.
Early assessment can help prevent minor issues from becoming chronic.
Horses are constantly exposed to moisture, insects, dirt, allergens, and changing weather conditions. These factors can contribute to weakening the skin’s natural barrier and making it easier for irritation, infection, or allergic reactions to develop. Most frequently seen on the body like the legs, mane, tail, and face.
It is case dependent on your horse. In some cases, pasture access may need to be modified or changed, as grasses can act as dietary triggers for certain horses. This will depend on your horse’s history and symptoms. PetDerm’s team will review in your consultation what is resonable and accessible for you and your horse, if an elimination diet trial is suggested.
Currently, there is no single blood or skin test that can reliably diagnose food allergies in horses. The most accurate method is a carefully managed elimination diet followed by controlled reintroduction of foods to identify the trigger. The PetDerm can provide guidance on an elimination trial while providing immediate support to your horse’s gut health.
Yes. A horse can develop a reaction to a food they have previously tolerated well. Over time, the immune system may begin reacting differently to certain ingredients, leading to new or worsening symptoms.
Immunotherapy works by gradually desensitizing the immune system to identified allergens, helping reduce the severity of allergic symptoms over time.
-
Long-term control of allergic skin disease
-
Reduced reliance on symptomatic medications
-
Improved comfort and quality of life
-
Management tailored to Alberta’s environmental allergens
Immunotherapy is particularly beneficial for horses requiring ongoing allergy management and those with limited response to standard treatments.
Horses with environmental allergies may show a wide range of symptoms, including:
-
Persistent or seasonal itching
-
Hair loss or broken hair coat
-
Skin thickening or pigment changes
-
Recurrent hives (urticaria)
-
Crusting, scabbing, or oozing lesions
-
Secondary bacterial or fungal infections
Because these signs can overlap with other skin conditions, accurate diagnosis is essential before initiating long-term therapy strategy.
Calgary’s PetDerm internal medicine vet is a board-certified Veterinary Internist. They complete an additional 4 years of dermatology or internal medicine residency before they become board-certified. The residency program involves extensive training in anatomy, physiology, pathology, clinical diagnosis, research, and more. A board-certified veterinarian dedicates at least 10 years to education and residency, similar to a doctor in human medicine.
A pet Internal Medicine specialist is trained in diagnosing and treating a broad spectrum of internal health issues in animals. They are highly trained and experienced in managing gastroenterology, endocrinology, infectious disease, urology, nephrology, respiratory medicine and hematology & immunology. It is common for a patient’s disease to impact multiple organs, requiring a detailed understanding on how to balance multiple issues for the best quality of life.
Whether it’s endocrine disease, gastrointestinal troubles, autoimmune problems, or chronic organ disease, our team works closely with your primary-care veterinarian to provide thorough diagnostics, personalized treatment plans, and ongoing support.
It’s easy to assume snoring or noisy breathing is “normal” for short-nosed dogs, and BOAS is often missed until it becomes advanced. The RFGS provides:
- An objective way to classify breathing ability
- Early detection of airway obstruction
- A clear guide for whether surgery would help
- A baseline to track improvement after treatment
Clinics using RFGS can confidently determine whether a dog would benefit from procedures like laser BOAS surgery, and how urgently.
The RFGS is a standardized way to measure how well a brachycephalic dog can breathe. It was developed by experts at the University of Cambridge to provide a consistent, objective way to diagnose BOAS and determine how severe it is.
It helps identify dogs who need treatment before they reach a crisis stage.
The RFGS includes two main parts:
-
Listening to breathing at rest
The veterinarian listens for signs like snoring, wheezing, stridor (high-pitched breathing), or excessive panting. -
A short, controlled exercise test
Your dog walks or trots on a lead for a few minutes (usually around 3 minutes).
After the walk, the veterinarian evaluates your dog’s breathing again — checking recovery time, airway noise, and effort.
This gentle test is safe and designed to mimic normal activity your dog would experience at home. A pre-screen chest x-ray may be required.
After surgery, rest and limited activity are essential. Monitor your pet’s breathing, attend follow-up visits, and follow all post-operative care instructions. Dogs often experience less pain and recover faster after laser surgery. Post-surgery Phovia Treatment may be offered to further expedite safe, bacteria-free healing.
Only Grade 0 dogs are considered BOAS-negative. Grades 1–3 are BOAS-positive with increasing severity.
In North America, there are common breeds that have a higher incidence of BOAS due to exterme brachycephalic anatomy:
- French Bulldog
- English Bulldog
- Pug
- Boston Terrier
- Pekingese
- Shih Tzu
These breeds can experience BOAS if their individual conformation is more extreme (i.e short muzzle, narrower nostrils, and elongated soft palate):
- Boxer
- Cavalier King Charles Spaniel
- Lhasa Apso
- Brussels Griffon
- Japanese Chin
Your family veterinarian may start by gathering a detailed history about your dog’s breathing habits – snoring, snorting, tiring quickly, heat intolerance, regurgitation, or noisy breathing. They will perform a full physical exam.
If BOAS is suspected, ask your family veterinarian to refer your pet to PetDerm. Dr. Becky Valentine does a detailed assessment using the Respiratory Function Grading Scheme (RFGS).
Even after successful surgery, long-term care is vital. Maintain a healthy weight, avoid overheating, encourage hydration, and engage in gentle exercise. These steps help prevent recurrence and support lasting respiratory health.
Over time, BOAS can lead to other health issues as a dog is working much harder to move air. Some conditions may appear alongside BOAS:
- Weakening of the voice box (laryngeal collapse) – When a dog struggles to breathe for a long time, the cartilage in the throat can weaken and start to collapse inward, making breathing even harder.
- Lower airway collapse (bronchial collapse) – If the upper airway becomes very compromised, the smaller airways deeper in the chest can also start to narrow or collapse.
- Digestive issues – Dogs with BOAS often swallow more air when trying to breathe, which can lead to problems like reflux, vomiting, or even a sliding stomach (hiatal hernia). Many of these digestive issues often improve once their airway is corrected.
- Aspiration pneumonia – Because breathing and swallowing become more difficult, there is an increased risk of food or liquid accidentally entering the lungs, which can cause a serious infection.
Common symptoms include loud snoring or breathing, exercise intolerance, gagging or coughing, cyanosis (bluish tongue or lips), and heat intolerance. Recognizing these signs early is crucial as untreated BOAS can progress to severe respiratory distress in up to 40% of cases.
Endoscopy is a minimally invasive procedure where a tiny camera is inserted into your pet’s digestive or respiratory tract to see inside and take tissue samples (biopsies) if needed.
Endoscopy helps veterinary internists diagnose causes of vomiting, diarrhea, weight loss, coughing, or difficulty swallowing. It’s often used to identify inflammation, infections, or foreign objects.
Yes. Endoscopy is generally very safe. It avoids the need for major invasive surgery and usually involves light sedation.
Endoscopy is a less invasive procedure, has a faster recovery time, causes less discomfort, and reduces the risk of complications compared to open surgery.
Most pets can go home the same day, though the PetDerm team may recommend a short observation period depending on their health and the procedure performed.
Visual findings are often available immediately. If biopsies are taken, results typically come back in a few days. PetDerm’s veterinary internist will discuss the samples and testing timelines with you prior to the procedure.
Yes. Veterinary X-rays use very low radiation levels, and exposure is kept to the minimum necessary to get a clear image.
Usually, no special preparation is needed. The PetDerm team will let you know if fasting is required if sedation is planned for. A team member will discuss this with you when booking the diagnostic procedure.
Most X-rays are quick—often just a few minutes. It may take longer if multiple views are needed or if your pet requires sedation.
Images will be reviewed by a veterinary radiologist for a more detailed report and PetDerm’s veterinary internist will follow up with you.
Yes. When indicated, we can perform ultrasound-guided fine needle aspirates (FNA) or biopsies to obtain tissue or cell samples for further diagnostic testing.
Cytology involves collecting cells using a fine needle and examining them under a microscope. This is minimally invasive and provides rapid preliminary information about the nature of a mass or organ change—whether it is inflammatory, infectious, or potentially neoplastic.
A fine needle aspirate (FNA) is performed using a thin needle, often without the need for general anesthesia, to collect a small number of cells from an organ or lesion. This is useful for screening and staging, particularly in cases involving the liver, spleen, lymph nodes, or abdominal masses.
Preliminary findings are often discussed the same day, with a detailed interpretation provided shortly thereafter by our board-certified veterinary radiologist.
Most ultrasounds take 30–60 minutes, depending on the complexity of the case and whether additional procedures (such as fine needle aspirates) are needed.
Yes. The area of interest is shaved to allow the probe to make direct contact with the skin and achieve the clearest images.
Fasting for 8–12 hours is typically recommended to reduce interference from gas in the intestines. Water is generally allowed. Specific preparation instructions will be provided by a PetDerm technician when your appointment is scheduled.
Yes. Ultrasound does not use radiation and is considered safe, lower risk procedure. Most pets do require sedation to allow for precise imaging position.
Ultrasound is a non-invasive imaging technique that uses sound waves to create real-time pictures of your pet’s internal organs. It helps assess their structure and detect abnormalities without surgery.
PetDerm’s Cancellation Policy
First Consultation: due to the high demand for appointments, PetDerm requires a deposit on file with booking your first consultation. Any rescheduling or cancelling of a first consultation within less than 3 business days will result forfeit of the deposit.
PetDerm will attempt to confirm your first consultation within 2 weeks of the appointment. We will try multiple times via email and phone number on file. If you do not confirm your appointment within 3 business days of the consult then it will be cancelled and the appointment slot will be provided to a waitlist patient. The deposit on file will be forfeited.
Recheck, Telehealth and RVT Recheck Appointments: PetDerm requires 3 business days for cancellations or rescheduling. If you provide less than 3 business days in either of these events a cancellation fee ($70) will be applied to your account.
PetDerm will attempt to confirm your appointment by email within 2 weeks of the appointment. If you do not confirm your appointment within 3 business days of the appointment, then your appointment will be forfeited and provided to a waitlist patient.
Procedures: PetDerm requires 3 business days for cancellations or rescheduling. If you provide less than 3 business days in either of these events a cancellation fee ($150) will be applied to your account.
Yes! Our goal is to help you manage your pet’s condition at home with the proper medications, diet, and monitoring tools. We provide guidance on at-home care and adjust treatments as needed based on regular check-ups.
Yes! We request medical history from your primary veterinarian(s) and you. A complete history will help us make the best recommendations. Please complete the New Patient Intake before you visit.
If you are the pet’s primary caregiver, it’s important that you’re here for the first internal medicine consultation so that we have the most information possible, and we can walk you through the initial options for your pet. When we meet, we’ll review past medical records, then our veterinary internist will perform a full exam. Together, we will develop a management plan. This consultation is just the beginning of our relationship — additional visits may be required throughout your pet’s journey towards improved comfort and quality of life.
Learn more about what to expect from your first visit.
Our Library is ever growing with resources. You can start your search with symptoms or diagnosis your pet may have.
Many pet insurance plans cover chronic disease management, but coverage varies by provider and policy. It’s important to understand how pre-existing conditions are covered under your pet insurance policy. If you’re looking into insurance, take time to review each provider’s coverage. We recommend checking with your insurer to confirm what’s included.
Most monitoring tests, such as bloodwork and blood pressure checks, can be done during a routine appointment. Some testing may require a short stay when diagnosing or trending response to therapy for certain diseases such as Cushings disease.
The frequency of visits depends on your pet’s condition. Some pets need monthly check-ups, while others require quarterly or bi-annual visits. Your veterinary internist will develop a personalized monitoring plan tailored to your pet’s specific requirements
Your perspective and input on your pet’s condition are of utmost importance for effective monitoring. In addition to physical examinations, use a combination of diagnostics to manage the underlying condition may include:
✔ Bloodwork and Urinalysis to trend underlying conditions
✔ Blood pressure monitoring
✔ Glucose checks for diabetic patients
✔ Outpatient Imaging (X-rays, ultrasound) when needed for further assessment
Stable medical management is designed for pets with chronic but non-urgent conditions that require ongoing monitoring and treatment. These conditions are not emergencies but still require regular veterinary internist oversight to ensure the condition is well-controlled and your pet has quality of life.
We suggest using luke warm water, not hot water to avoid further irritating or drying out your pet’s skin. Luke warm water can help soothe and clean without causing further discomfort.
Avoid bathing areas with open sores or wounds. Consult your veterinary dermatologist for the best approach to care for these sensitive spots.
We understand that shampoo therapy may not be feasible for every pet owner due to physical limitations, time constraints, or concerns about their pet’s behavior during bath time. These challenges are common and valid. If you have reservations or uncertainties about bathing your dog, please communicate with the PetDerm team about it. PetDerm is here to support you and your pet’s well-being by offering in-house medicated bathing services. Our experienced staff love giving your pet the spa time they deserve!
A consultation with PetDerm’s veterinary dermatologist can help you find the best product for your pet. Through an examination and assessment of symptoms, along with the diagnostics of cytology, they can determine the right combination of ingredients to soothe and repair your pet’s skin barrier.
Medicated shampoos not only cleanse the skin and coat but also contain additional therapeutic ingredients. These may include antimicrobial agents to reduce bacteria and yeast, anti-itch or anti-inflammatory components to improve comfort, moisturizers and emollients to help repair the skin barrier, and anti-seborrheic ingredients to relieve dryness and flakiness.
After the otoendoscopy procedure is complete, Petderm’s veterinary dermatologist will discuss the findings and a personalized treatment plan. While it is uncommon to have any post-op care, there will be follow up required.
The procedure itself is not painful but if your pet is experiencing an active ear infection there may be more associated discomfort. Otoendoscopy is general done under general anesthetic and any pain or discomfort is managed by PetDerm’s veterinary dermatologist and team.
Certain medications and therapy may interfere with the results of intradermal testing. These medications must be withdrawn accordingly prior to the procedure. Please contact your family veterinarian to discuss safe withdrawal from any of these medications.
Medications mostly commonly used in allergic patients that would interfere with intradermal testing:
- Oral, injectable or topical steroids and anti- histamines.
Medications most commonly used in allergic patients that DO NOT interfere with intradermal testing:
- Oclacitinib (Apoquel), Lokivetmab (Cytopoint), Ilunocitinib tablets (Zenrelia), Cyclosporine (Atopica).
Immunotherapy (allergy shots (SCIT) or allergy drops (SLIT)) consists of giving microdoses of the allergens your pet is allergic to, to your pet, over time. We slowly increase the dose and aim to create immune tolerance for your pet. Over time, it trains your pets immune system to become desensitized to the allergens.
Cytology is a diagnostic test that is simple and easy to obtain from most pets. Cytology of the skin or ear is used to identify inflammation and the type of infection present. To perform a cytology test, a PetDerm nurse will use a swab, tape, or slide to collect samples from the ear, which will be examined under a microscope for diagnosis.
The most visible and common symptoms are itchiness toward the affected ear, scratching or rubbing the ear and head shaking. In some cases, excessive debris within the ear, material draining from the ear or an odor might be present. The ear may be red, swollen or scaly.
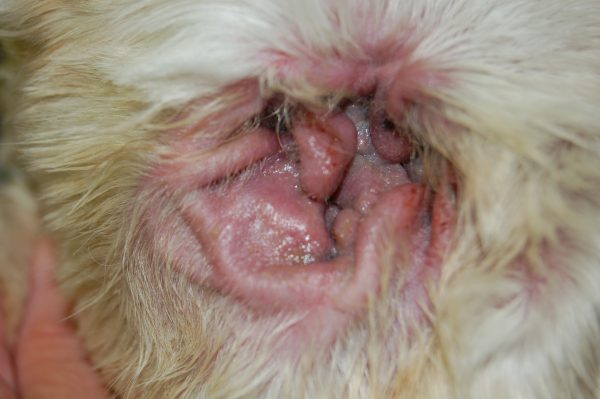
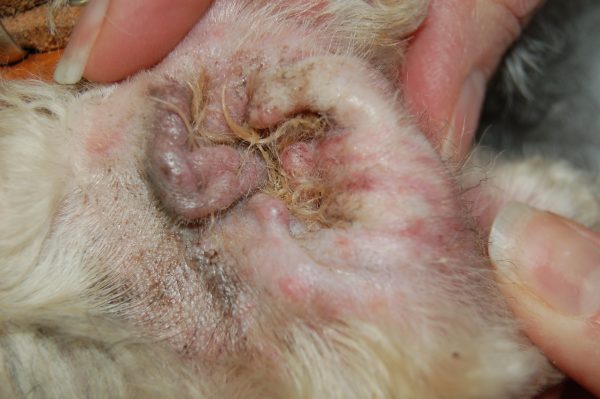
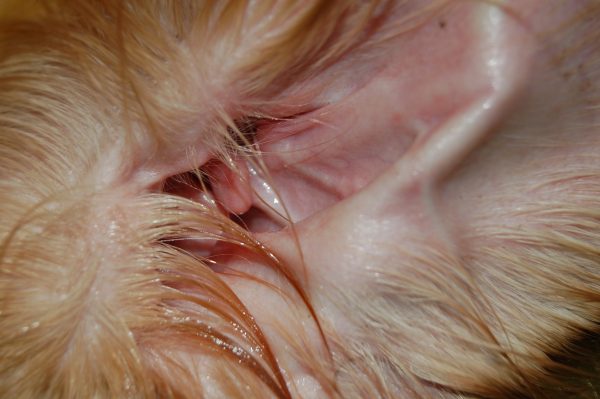
Most common symptoms of an allergy include itching, scratching, head flapping and excess licking. Often dogs and cats will experience inflammation of their skin and ear and often experience recurrent and chronic secondary skin and ear infections.
If your pet is experiencing environmental allergies, their symptoms may be seasonal, and change throughout the year. If your pet has concurrent or undiagnosed food allergies, which may occur alongside environmental allergies, they may experience gastrointestinal symptoms such as soft stools, diarrhea, increased bowel frequency, and vomiting.
Allergy testing is not recommended under 1 year of age. In some cases, we may even recommend waiting longer.
PetDerm’s Library is ever growing with resources. You can start your search with symptoms or diagnosis your pet may have.
Yes! Even though pictures say a thousand words, the skin and ears need to be viewed and assessed in-person. We would need to meet you and your pet to determine the most probable diagnosis and treatment plan.
For dermatology patients, if you and your family veterinarian suspect a diagnosis of atopic dermatitis, PetDerm can schedule the consultation and allergy testing on the same day. Please note that more than one visit will be required to help you and your pet.
Start the process today by asking your family veterinarian for a referral today!
You can find a list of veterinary dermatologists and internists in Canada to locate the one nearest to you!
Expect to be at PetDerm for approximately 60 minutes. If you did not fill out the New Patient Intake form, please arrive 15 minutes early to fill out the form.
Allergy testing for dogs can be done by intradermal allergy test (intradermal skin test) or by blood test. The intradermal test is considered the most reliable. For the intradermal test, dogs are typically lightly sedated (not under general anesthesia), a patch of hair is clipped on the side of the chest and multiple allergens are injected into the skin. Reactions are measured and recorded.
Each pet is different, depending on the severity of disease and infection, your pet may require sedation or anesthesia. A consultation with PetDerm’s veterinary dermatologist will determine the best approach for your pet’s comfort and safety.
Yes! We ask you to fill out our New Patient Intake that is detailed record of your experience of your pet’s symptoms. Please set aside 10 to 15 minutes to complete the intake. Also, we request medical history from your primary veterinarians(s) and you.
An elimination diet trial is the only accurate and reliable method to identify a food allergy. Intradermal allergy testing, blood testing and saliva/hair all produce unreliable results, please make an informed decision if you proceed with these tests.
At this time, there is no reliable at-home allergy test on the market. While they are available (using your pet’s hair or saliva), they are not validated nor tested against conventional allergy tests. Most importantly, they don’t provide you an accurate diagnosis nor with a solution for long-term allergy management.
For food allergies, unfortunately, no blood, hair or saliva test has been shown to reliability diagnosis adverse food reactions. Currently, the only reliable diagnostic test for food allergies is an elimination diet trial.
Watch this YouTube video from DVM360 to learn more about debunking at-home allergy tests.
Otoendoscopy is considered a generally safe procedure but like any medical procedure, there may be minimal risks. There are associated risks if you pet requires sedation or anesthesia for this procedure. A PetDerm team member will discuss these risks and your concerns prior to the procedure.
Many pets show signs of improvement after just a few sessions. The exact timeline can vary depending on the condition being treated and the individual pet.
Yes, Phovia can be used in conjunction with other treatments. It is often used to complement other therapies to enhance overall healing and recovery.
No, Phovia treatments are painless and non-invasive. Your pet should not feel any discomfort during the session.
A typical Phovia treatment session lasts about 10-15 minutes, making it a quick and convenient option for pet parents.
The frequency of treatments depends on the specific condition and its severity. Typically, Phovia treatments are administered weekly until the condition improves.
Yes, Phovia is safe for both dogs and cats. It is a non-invasive, topical treatment that promotes natural healing without the need for additional medications like antibiotics.
Phovia can be used to treat a variety of skin conditions, including:
- Hot spots
- Bite wounds
- Lesions from continuous licking
- Traumatic wounds
- Skin infections
- Surgical incisions.
Phovia Fluorescent Light Therapy is a treatment that uses fluorescent light energy to accelerate the natural healing process of your pet’s skin. It is effective for various dermatological conditions in both dogs and cats.
Phovia works by emitting fluorescent light that penetrates the skin to stimulate cell regeneration. This helps in faster healing of wounds, infections, and other skin conditions. Often reduces healing time to half.
Vetoquinol has an informative pet owners information and video explaining how the Phovia works. Click here to learn more!
Blood and urine tests in animals offer insights into various body systems, including liver and kidney function, anemia, and thyroid function. These laboratory tests provide valuable internal information that may not be evident externally. Periodic blood and urine tests can even detect early disease processes before outward symptoms emerge. While urine testing (urinalysis) is not superior or inferior to blood testing, it complements it, offering a more comprehensive understanding when both are combined.
Yes, absolutely! Ringworm (dermatophytosis) can indeed be a contagious infection, and in certain instances, it can transfer from cats or dogs to their human companions. However, the likelihood of transmission varies depending on the specific type of infection, the areas affected on the pet, and the individual susceptibility of the person. Given that other infections may resemble ringworm, it is crucial to achieve an accurate diagnosis of dermatophytosis before initiating treatments for the pet or the pet owner.
Dermatophytosis, commonly known as ringworm, is a fungal infection affecting hair, superficial skin, and occasionally nails. It is caused by three fungal organisms: Microsporum canis, Microsporum gypseum, and Trichophyton mentagrophytes. Sources of infection include infected pets, rodents, contaminated environments, and sometimes the soil. While less common, dermatophytosis is contagious and zoonotic, potentially transmissible to humans. Diagnostic methods include fungal culture, PCR testing, skin biopsy, and, in some cases, identification of fungal spores in impression smear cytology. A woods lamp examination can heighten suspicion. Treatment requires thorough care, extending beyond clinical cure, with a repeated fungal culture to confirm complete resolution typically performed.
Trichogram, also known as trichography, involves the microscopic examination of hairs. In this procedure, hairs are plucked, placed in mineral oil, and examined under a microscope. When assessing hairs from an animal with skin or hair coat issues, a veterinary dermatologist can identify evidence of infection, trauma, or hair malformation. Additionally, this method may reveal parasites such as Demodex residing within the hair follicle.
Skin scrapes involve using a dulled scalpel blade to collect material from the skin surface for microscopic examination. These scrapes are crucial for detecting parasites, particularly Demodex mites, which cause inflammation, hair loss, scaling, and secondary infections.
Deep skin scrapes focus on identifying mites living within hair follicles. This requires a small area and leaves a superficial abrasion. Superficial skin scrapes cover a larger area, collecting surface crust and skin cells to identify Sarcoptes and other surface mites that cause inflammation and itching.
Detecting mites through skin scrapes can significantly impact treatment, leading to a faster resolution of skin issues and relief from discomfort.
Cytology is a less invasive test than biopsy. Cytology entails collecting material from a specific patient, often from the surface of the skin or other lesions. In contrast, a biopsy involves obtaining a small tissue piece from a diseased area, submitting it for processing, and having it examined by a histopathologist. Petderm’s Dermatologist Veterinarian conducts in-house cytology, providing results during your examination.
Cytology revolves around collecting material from a specific patient and examining it under a microscope. The accuracy of this process hinges on the nature of the disease or problem being assessed, the type of sample obtained, and most crucially, the experience of the observer. Notably, experienced dermatologist vets excel in reading cytology slides, enhancing the accuracy of diagnoses. For instance, while cytology is highly effective in diagnosing bacterial or yeast infections, it may not be the preferred diagnostic tool for identifying skin cancer.
Cytology, encompassing impression smear cytology and diagnostic cytology, is a non-invasive procedure involving the collection of samples from a patient for microscopic examination. Material is obtained using a cotton swab, tape, or other instruments, then examined under a microscope to provide valuable insights into specific issues. This process aims to uncover evidence of infections, types of inflammation, immune-mediated diseases, or neoplasia. Experienced veterinary dermatologists, including clinical pathologists at outside labs or in-house specialists, often perform cytology, ensuring accurate and detailed analyses of the obtained samples.
Cytology, whether in the form of impression smear cytology or diagnostic cytology, stands as a non-invasive and highly valuable method, particularly in the diagnosis and reassessment of skin and ear diseases. This technique involves acquiring patient samples for microscopic examination and furnishing crucial information and evidence for specific issues. In the realm of skin and ear diseases, cytology proves especially advantageous for diagnosing infections and can also play a role in the initial assessment of certain immune-mediated diseases and specific types of cancer.
PetDerm advises pet parents to try to keep their pet calm and inactive during the day and evening following a surgical procedure. The timing for a pet’s return to normal activity and habits may vary, and it is recommended to follow the specific medical advice provided for your pet after the procedure.
Potential side effects or complications from CO2 laser surgery are uncommon and the same as with any surgery. These may include swelling, discomfort or pain at the surgery site, and, very rarely, secondary postoperative infections. These events are uncommon and happen less often than with conventional surgical techniques.
CO2 laser surgical procedures generally entail less pain and swelling compared to traditional methods. While sedation or general anesthesia is commonly required, recovery after CO2 surgery is typically swift.
The recovery time varies based on the type of surgery, but overall, recuperation tends to be swifter after CO2 laser surgery in comparison to traditional surgical procedures. PetDerm offers Phovia Light Therapy to further expedite the healing process.
CO2 laser surgery utilizes a carbon dioxide laser instead of conventional instruments like scalpel blades for various surgical procedures. The use of a CO2 laser offers several advantages, including reduced pain during recovery, minimized inflammation, and faster recuperation. Particularly when removing surface lesions or growths, the CO2 laser allows for the excision of multiple masses without the need for suturing each site. This not only streamlines the surgical procedure but also contributes to a more efficient and expedited recovery process. PetDerm offers Phovia Light Therapy to further expedite the healing process.
Skin biopsy involves obtaining a small sample of skin or a skin lesion to gain detailed insights into specific diseases, infections, growths, or tumors. This diagnostic procedure is particularly valuable for addressing challenging or deep-seated infections, immune-mediated diseases, and distinguishing between benign and malignant growths. Its versatility makes it a crucial tool for meeting various diagnostic needs, providing comprehensive information to guide effective treatment.
The detailed information obtained from the biopsy is instrumental in ensuring the correct diagnosis, allowing for tailored and effective treatment plans. In cases where diagnostic clarity is essential, a skin biopsy proves to be an invaluable tool for veterinary dermatologists and internists in providing optimal care for their patients.
A skin biopsy is usually painless. Before conducting the biopsy, the pet is sedated, and a local anesthetic is injected just below the skin at the biopsy site. This ensures numbness of the area, which can last for 2-3 hours after the procedure.
A skin biopsy is generally a quick procedure, with the exact duration varying based on factors such as the number and location of sites being biopsied and the speed of sedation for the individual. The typical timeframe for the procedure can range from 30 minutes to 2 hours.
Biopsy results typically require 2-4 weeks to be processed. After obtaining samples, they are preserved and sent to a laboratory for processing and tissue staining. Subsequently, the samples are sent to a dermatopathologist* for thorough review and analysis. Once the dermatopathologist records their findings, they are shared with the veterinary dermatologist for further review and decision-making regarding treatment. In certain instances, special stains or advanced analysis may be necessary, extending the processing time.
*A dermatopathologist is a veterinary specialist combining expertise in both dermatology and pathology to accurately identify skin conditions through tissue analysis. They work closely with dermatologist veterinarians to interpret biopsy results and make diagnoses.
Commonly, biopsies result in minimal side effects, such as itching or pain at the biopsy site, as well as potential swelling or bleeding. In the event of severe instances of these effects, pet parents should contact PetDerm immediately or their primary veterinarian if it is outside of PetDerm’s business hours.
As a precautionary measure, it is recommended that pet parents keep biopsy sites covered or have their pets wear an Elizabethan collar (“cone of shame”) or medical pet shirt until sutures are removed to prevent any potential trauma to the biopsy site.
When scheduling a biopsy, pet owners are advised to have their animals fast the night before, as sedation or anesthesia might be required. Additionally, they should refrain from cleaning, bathing, or applying medication to the skin lesions being sampled. A PetDerm team member will provide you with more details upon booking the biopsy.
It is not recommended to use raw food for an elimination diet trial. Raw diets can pose health risks due to potential contamination with harmful bacteria like Salmonella and Listeria. These bacteria can make both pets and their owners’ sick. For a safe and effective elimination diet, it’s best to use a specially formulated commercial diet or a home-cooked diet prepared under the guidance of a veterinarian.
Food allergies may appear in dogs and cats at almost any age. Studies show, however, that food allergy is more likely than environmental allergy to appear in very young animals (less than 6 months) and in older animals.
Food allergy is a genuine allergic response where the immune system becomes overly sensitive to ingredients a pet has previously eaten. For food allergy to occur, the pet must have been exposed to the problematic allergen or a similar one with cross-reactivity. On the other hand, food intolerance doesn’t need prior sensitization and can happen on the first exposure. In dogs and cats, food intolerance reactions typically manifest as gastrointestinal issues like diarrhea or vomiting.
An elimination diet for a cat or dog involves feeding them a special diet that excludes all the ingredients they have previously eaten. This helps identify which foods might be causing allergies. The process typically lasts for at least 8 weeks, but it can extend up to 12 weeks. During this time, it’s crucial to avoid giving your pet any treats, chews, or flavored medications that could interfere with the trial. If symptoms improve, potential allergens are reintroduced one at a time to pinpoint the specific cause of the allergy. The PetDerm team can help you develop an elimination diet to improve your pet’s quality of life.
The only reliable way to diagnose food allergies in dogs and cats is through a strict elimination diet trial. While some tests claim to detect food allergies using blood, hair, or saliva, they are not reliable or dependable.
Symptoms of food allergies in dogs and cats may include behaviours such as licking, scratching, chewing, and rubbing various regions like the face, ears, rear, armpits, and other body parts. Additionally some pets with food allergies may present gastrointestinal manifestations such as loose stool and vomiting. Distinguishing food allergies from environmental allergies can be complicated and that is why we are here to help. Diet consultations with a veterinary dermatologist can help your pet enjoy food again!
If an ear infection is left untreated, it is likely the infection will continue and worsen. In severe cases, the infection may cause rupture of the ear drum and progress to a middle ear infection. If you have experienced an ear infection, you’ll relate to how uncomfortable and in some cases, painful it can be. Ear infections should be addressed when you first notice symptoms to minimize the impact to your pet.
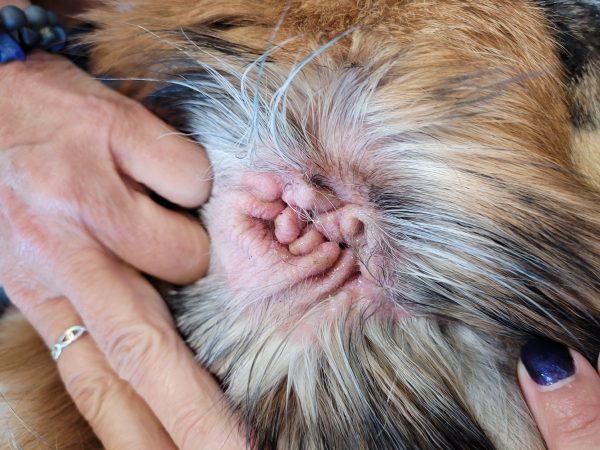
There can be a variety of causes for ear problems including underlying allergies, polyps, tumors, chronic infection and underlying endocrinopathies. The most common cause is underlying allergies that trigger inflammation, itch and secondary infections. PetDerm’s veterinary dermatologist and team specializes in the diagnosis and management of challenging and recurrent ear problems.
Serum allergy test is less invasive than the skin test. It is very important this test be done at the right time for each pet – if the test is run at the wrong time it may be negative despite the patient being allergic. This blood is taken in-clinic and the test is done at an outside lab. The only reason to do allergy testing in a pet is to use the results to begin immunotherapy and desensitize your pet to their environmental allergies.
Atopic dermatitis in dogs and cats is a chronic, inflammatory skin condition caused by sensitivities to environmental allergens such as pollens from trees, weeds and grasses, common dust mites, or mold. It often results in itching, redness, hair loss, and skin and ear infections.
Diagnosis involves a combination of history, clinical signs, and ruling out other skin conditions. Accurate diagnosis is crucial for managing symptoms and improving the quality of life for pets with this condition.
Learn more about Atopic Dermatitis and it’s symptoms, on the Empathy for Itch initiated by The Canadian Academy of Veterinary Dermatology (CAVD).
If you’re the pet’s primary caregiver, it’s important that you’re here for the first dermatology consultation so that we have the most information possible, and we can walk you through the initial choices for your pet. When we meet you and your pet, we’ll review your pet’s medical records, then our dermatologist vet will do a full exam which can include using tools to take a better look at what we can’t see. Together, we will start the building blocks of a management plan. This consultation is just the beginning of our relationship — the first of many visits throughout your pet’s journey towards improved comfort and quality of life.
Because allergies are incurable, it can be frustrating to try things and not see results. As dermatology and allergy experts, we bring more resources and accurate testing to the table, which can lead to much better outcomes. Visit our library to understand how better outcomes from visiting a Veterinary Dermatologist.
Allergies can be managed, but rarely cured, and we’re committed to being a successful part of your pet’s allergy journey.
Food allergies account for up to approximately 30% of pets with allergies, but they can be layered with allergies to house dust mites, pollens, grasses, and trees, which makes it hard to treat with diet alone. And because there is no accurate food allergy testing available in veterinary medicine, a change in diet might only work when addressing other factors that could be causing your pet’s rash, itch, or ear infection.
The goal of allergy testing is not to ‘diagnose’ an allergy in your pet. A diagnosis is made with a dermatological history, a dermatological exam, ruling out other causes of itching, and coming to the clinical diagnosis of Atopic Dermatitis – or hypersensitivities to environmental allergens. Once the diagnosis is made, the purpose of the allergy test is to formulate an immunotherapy for your pet. Immunotherapy (allergy shots (SCIT) or allergy drops (SLIT)) consists of microdosing your pet with what it is allergic to over time. This will create immune-tolerance where your pet gets used to the allergen and the symptoms are reduced or resolved.
Our allergy testing is done by looking at your pet’s immune response to particular environmental allergens. There is no accurate food allergy testing available in veterinary medicine which means our tests looks for environmental allergens only. There are 2 ways to perform allergy testing:
Intradermal skin test: in some ways the most accurate test. This test is done under light sedation, followed by the injection of over 50 different allergens in between the layers of the skin (intradermal). The allergens that are causing reactions (wheals- or large bumps) are the ones we identify as triggers for your pet.
Serum allergy test: This is less invasive than the skin test. It is very important this test be done at the right time for each pet – if the test is run at the wrong time it may be negative despite the patient being allergic. This blood is taken in-clinic and the test is done at an outside lab. We recommend you speak with a veterinary dermatologist before you have any serum test done.
If you’re concerned about lesions on your pet’s body, itching, or secondary infections, please see your family veterinarian. If care is needed outside of business hours, see an Emergency Veterinarian.
If your pet is stable but uncomfortable, a cool soothing bath can alleviate some discomfort. You can use cool cloths and gentle shampoos. Treats help too.
Explore Equine Services


